With nearly 2.5 million Americans said to be addicted to prescription opioids or heroin, there is no doubt that we are in the midst of an epidemic involving addiction to painkillers.
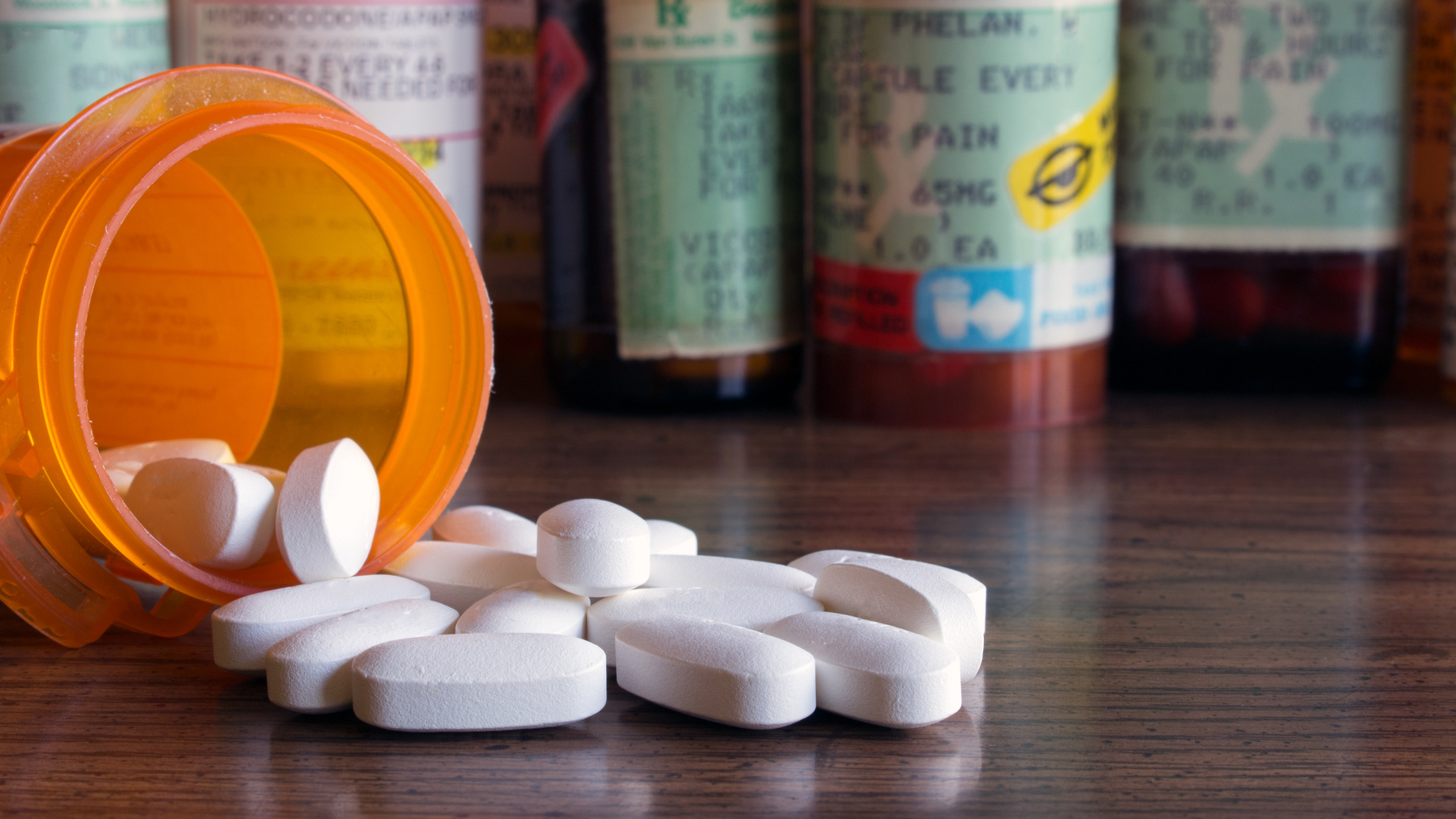
We Worked with 4 Patients Who Were Dealing With Opioid Dependence and Here’s What We Found
It has become almost a weekly occurrence that we hear about the opioid addiction crisis that is taking a toll on Americans throughout the country.
The White House has declared the nation’s opioid epidemic a public health emergency, and part of the plan to address the epidemic on the federal level will now include more research and development and an awareness campaign aimed at scaring kids away from the abuse of prescription drugs.
We know there is a crisis, but let’s take a look at the facts from a doctor’s perspective:
- Since 1999, sales of prescription opioids in the U.S. have quadrupled.
- From 1999 to 2015, more than 180,000 people died from overdoses related to prescription opioids.
- Nearly 2 million Americans abused or were dependent on prescription opioids in 2014.
- An estimated 1 out of 5 patients with non-cancer pain or pain-related diagnoses are prescribed opioids.
- Many doctors are concerned about their patients becoming addicted to painkillers but are not always equipped to safely manage these patients’ pain.
Looking at the data that we know and what we often hear about the opioid epidemic, one might think that a solution is still out of reach. But is it really?
We know that while doctors who prescribe opioids to patients have become more of the focus of this epidemic, most doctors are following the guidelines outlined by the Centers for Disease Control and Prevention when it comes to prescribing opioids for chronic pain.
In fact, those guidelines provide clear recommendations for the prescribing of opioid pain medication for patients 18 and older and they focus on the use of opioids in treating chronic pain (pain lasting longer than 3 months or past the time of normal tissue healing) outside of active cancer treatment, palliative care, and end-of-life care.
Here’s one fact that you probably won’t hear that much about: Managing chronic pain can be devastating. But patients can work with doctors to find safe and effective ways to treat pain.
It is with this last point that we want to share some hopeful news in the midst of this national health crisis.
The Tolbert Center works with many patients who are either dependent or addicted to opioids. Although we have numerous success stories, we want to share four cases we successfully weaned the patients off pain pills and helped them maintain a lifestyle free of painkillers right in the doctor’s office, without hospitalization.
The following examples show that, while the opioid epidemic seems like it is getting out of hand, there are a growing number of cases where people are getting the help they need to overcome opioid dependence and live normal lives.
Case No. 1
A 46-year-old martial arts enthusiast came to the center after getting hurt from being kicked in groin, which injured his nerves.
Fellas, just imagine being kicked in the groin and that pain never going away. That’s how this patient was describing his level of discomfort.
“Doc,” he told Dr. Tolbert. “I feel like my balls are on fire.“
After some initial tests and more tests and years of antibiotics, he still suffered. Eventually, the doctors told him there was nothing more they could do. On top of that, they said all his tests were normal.
Sadly, the patient still felt this burning pain in his pants, and he was placed on large doses of oxycodone daily, which provided relief but eventually took over his life and ruined his relationship with family, friends and work.
We were able to get him off the oxycodone using a Buprenorphine-Naloxone combination, also known as Suboxone. Suboxone is a partial opiate with a blocking agent.
After checking into our center at 8 o’clock in the morning, he spent the day participating in our programs, including support groups, and he was able to get off of his medication by the next day.
Although not for everyone, Suboxone is a great option for patients who want the quickest and most comfortable opiate-weaning option. Dr. Tolbert recommends Suboxone be used as part of our integrative treatment program. Suboxone, prescribed for opiate recovery and addiction, helps ease cravings and painful withdrawal symptoms, which may occur during rapid weaning.
Case No. 2
We met Pam, a 59 year-old active hiker and antique collector, over two years ago, She crawled into our office after hearing cracks and pops in her body followed by severe back pain during her routine chiropractic manipulation.
She had round-the-clock Fentanyl patches “glued” to her body due to her intense back pain.
Every day, she said she could only take about five steps before having to sit down again. (And that was on a good day.)
Not on the day she decided to come to the center
Pam has been off her initial pain medications for more than two years now and boasts of her active lifestyle.
How was she able to overcome her dependence on opioids? With a platelet-rich plasma (PRP) procedure.
“Here I am today, 60 years old and pain-free,” she wrote to Dr. Tolbert last year. “I am a large-scale antiques collector, and I am once again able to walk the miles-long weekend venues.”
“I did a movie recently, which required me to walk up a steep hill and fall head first into a well,” she continued. “And I was able to do it. A far cry from the me before you. Thank you, Dr. Tolbert, for giving me back my life.”
Case No. 3
In another case, we worked with a 42-year-old woman who said she was in desperate need of returning to the workforce so she could leave her husband and start a new life.
She was referred to the center by the local pain anesthesiologist, wearing a Fentanyl patch with Dilaudid after her nerve was injured during a surgical procedure.
Just to be clear, Fentanyl and Dilaudid are some of the strongest opioids known to man (they make Morphine look like Tylenol).
The patient was also taking medication for depression, and she was gaining weight. As you can imagine, it was “not a good look“ once she was ready for dating, she said.
It has been nearly two years since we worked with her, and she no pain or depression medications. She is also more independent now, working as a waitress. She also glows talking about her “hot” new man and her 30 pounds of weight loss.
How did she achieve these results? With one epidural, working with our pain psychologist, and supervised and prescribed exercises.
Case No. 4
Another patient, a 55-year-old teacher, came to the center after having been on disability and taking Norco daily for chronic low back pain and an Achilles tendon tear.
What were the results, you may ask? It’s been nearly two years, and the patient is no longer taking medications.
The patient was healed with prolotherapy and PRP specifically for the Achilles tendon and spine.
As you can tell from these examples, no one case of opioid dependence is the same.
But there are real solutions out there for patients who need access to safer, more effective treatments for chronic pain.
One of the best solutions we have found at the center for reducing the amount of deaths and abuse is to customize all treatments and prescriptions for each patient. It also remains true that it’s important to prescribe and supervise treatment for opioid dependence properly.
And if you’re ever wondering whether any of these patient success stories are true or whether they just came from one of your favorite medical TV dramas, look no further the California Department of Justice. All of these patient success stories were verified through California’s Prescription Drug Monitoring Program (CURES).
The Tolbert Center for Rehabilitation and Wellness is a Los Angeles-area state-of-the-art medical facility specializing in using non-surgical and minimally invasive techniques and procedures for the management of chronic pain. Dr. Glenna Tolbert, the founder of the center, is Board Certified in Physical Medicine and Rehabilitation, with a sub-specialty in Spinal Cord Medicine. Dr. Tolbert believes in a holistic approach to healthcare, where the physician, team of specialists and patients work in partnership to restore the quality of life to each patient. To learn how we’re putting the patient back at the center of health care, check out the Tolbert Center difference.
Comments (1)
Comments are closed.


[…] The easy thing to do would have been to prescribe the patient opioids. […]